Venous leg ulcers, also known as venous stasis ulcers or leg ulcers, are a medical condition affecting millions worldwide. Chronic open wounds can become recurrent and difficult to heal without proper medical care and management.
Typically, venous leg ulcers are painful and uncomfortable. It can also cause swelling, itching, and sensitivity to the affected area. This condition can also significantly impact the patient’s quality of life. Dealing with ongoing pain, wound care, and potential limitations on daily activities can often cause frustration and emotional stress.
This blog will discuss the causes, risk factors, and venous ulcer treatment options available for those who suffer from the condition. So, if you are wondering how to treat leg ulcers, this article has all the answers. Let us start with the causes of venous leg ulcers.
What Are Venous Ulcers And Their Causes?
Venous ulcers are open, long-lasting wounds that take weeks or months to heal. It usually develops on the legs, just above the ankle. It makes them significantly harder to deal with because they are prone to recur.
This condition occurs due to impaired blood circulation in the legs, also known as venous insufficiency. When the valves of the veins in the legs are damaged or weak, they cannot push the blood back up to the heart efficiently, causing blood to pool in the lower legs and feet. This can manifest as leg pain, heaviness, and swelling. If left untreated, venous insufficiency can worsen, resulting in varicose veins, deep vein thrombosis, and venous leg ulcers.
Venous leg ulcers develop due to the pressure increase and fluid buildup in the affected veins. The ongoing high pressure and pooling of blood lead to the breakdown of skin and the formation of open wounds or ulcers on the lower legs. If you are already dealing with varicose veins, where the blood circulation is abnormal, you must ensure that you do not cut or scrape yourself. This could also trigger an ulcer.
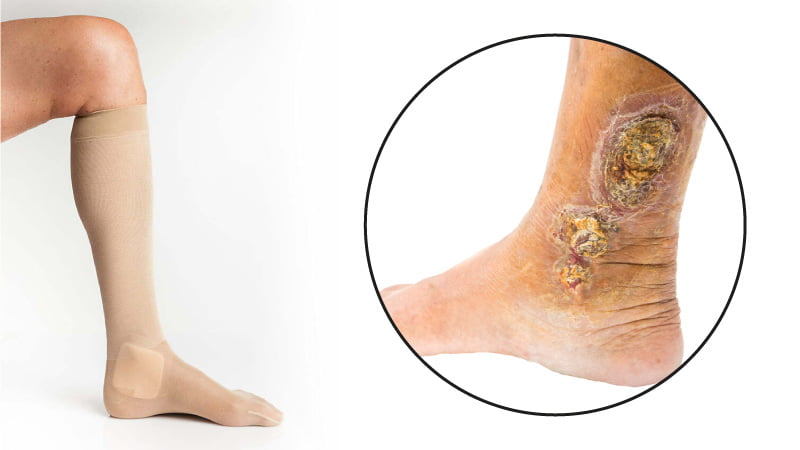
Who’s More At Risk Of Developing Leg Ulcers?
Some people are more susceptible than others to developing venous leg ulcers due to their medical history, lifestyle, and specific demographic characteristics. The following factors can increase the risk of developing venous insufficiency and, therefore, venous leg ulcers:
- Age: As you age, your vein valves weaken and cannot perform efficiently. Further in the blog, we have also mentioned the treatment for leg ulcers in the elderly that can be used to treat open wounds
- Gender: Women are more prone to developing venous conditions
- Sedentary Lifestyle: If your work requires you to sit or stand for long hours, you could be increasing your risk for venous conditions
- Family History: If your parents had a venous condition, you are more likely to develop them as well
- Pregnancy: Due to hormonal changes and pressure from the growing uterus, pregnancy can impact your veins
- Injury: An injury to the veins can leave them impaired
What Venous Ulcer Treatments Are Available?
This section will focus on how to treat venous ulcers. Venous ulcer treatments typically involve a combination of medical interventions. A vascular surgeon or wound care specialist will assess the specific situation and recommend the most appropriate treatment plan. Regular follow-up visits are essential to monitor progress and adjust the treatment plan as needed.
The treatment plan will include a combination of the following:
- Venous ulcer stockings or compression wraps
- Topical ointments
- Wound dressings and debridement
- Antibiotics
- Venous procedures such as sclerotherapy, radiofrequency ablation to treat the underlying venous insufficiency
- Other lifestyle changes such as regular exercise, the elevation of the affected leg, avoiding prolonged sitting and standing
How To Prevent The Recurrence Of Venous Leg Ulcers?
To prevent the recurrence of venous ulcers, one must address the underlying cause and the risk factors for the relapse.
- Wearing compression stockings regularly can help promote blood circulation in the legs, thus reducing the risk of ulcer formation. With the severity of the condition in mind, the doctor will determine the optimal compression level.
- Managing underlying medical conditions can reduce the risk of ulcer recurrence. Conditions such as venous insufficiency and diabetes should be controlled under your doctor’s guidance.
- Wear proper footwear and avoid injuries. Take precautions to prevent leg injuries, as even minor cuts or injuries can lead to complications in individuals with venous insufficiency.
- Avoid prolonged periods of sitting or standing. Staying physically active is a great way to boost blood flow naturally.
- Take care of your skin, moisturize them regularly, and avoid dryness. Monitor your legs for signs of skin color changes or ulcers. Early detection and prompt treatment can prevent the condition from worsening.
The Best Home Remedies To Effectively Manage Leg Ulcers
The following are some of the leg ulcer treatments a home that can be done alongside medical care:

- Maintain an Active Lifestyle: It is essential to have an active lifestyle to manage leg ulcers at home. Poor circulation in the lower extremities increases the chances of developing leg ulcers. Therefore, avoid sitting or standing for long hours at a stretch. When resting, keep your leg elevated, if possible. This can reduce swelling and promote blood circulation.
- Regular Exercises: Simple stretches and movements can help improve blood flow to the feet and ankles. Your physician will instruct you on how many stretching exercises you can perform to manage the edema and prevent blood pooling in the legs. Yoga, walking, and other low-impact exercises can promote healthy circulation in the lower extremities.
- Healthy Diet & Weight: Maintaining a healthy diet and body weight is essential to support your body’s natural healing process.
For leg ulcer healing and for managing venous ulcer wound care, a combination of medication, compression therapy, and lifestyle changes are recommended.
Conclusion
Venous leg ulcers are a severe complication of Chronic Venous Insufficiency. Therefore, not everyone with venous insufficiency will develop ulcers. The key to preventing the development of venous leg ulcers is early detection and correct management of venous insufficiency. Compression therapy, lifestyle modifications, and medical interventions can effectively treat venous insufficiency and reduce the risk of ulceration. If you have symptoms of venous insufficiency, it’s crucial to consult a doctor for a proper evaluation.
Frequently Asked Questions
Q1. What Is The Gold Standard For The Treatment Of Venous Ulcers?
The gold standard for the treatment of venous leg ulcers is compression therapy. Graduated compression must be applied to the leg using bandages, compression stockings, or compression wraps to help improve blood circulation, reduce swelling, and promote healing.
Other treatments may also be used, along with compression, to support wound healing and address factors contributing to venous ulcer development.
Q2. Are Venous Ulcers Wet Or Dry?
Venous ulcer wounds are usually wet with discharge. As a result, discoloration, swelling, and itching around the lesion are common.
Q3. What Food Is Good For Leg Ulcers?
A zinc-rich diet must be followed by patients suffering from venous leg ulcers. The diet must include eggs, chicken, pulses, green vegetables, etc.


Comments
There are no comments yet.